Following neurulation, the spinal cord runs the entire length of the trunk of the body. The cord extends to the coccyx, and all the spinal nerve roots are short and nearly horizontal as they course to their respective IVFs, with no cauda equina and no large lumbar cistern. As development proceeds, differential growth rates of the spinal cord, vertebral column, and trunk of the body cause the spinal cord to regress in length relative to the vertebral column. As a result, the conus medullaris shifts to higher vertebral positions, and the lower spinal nerve roots and filum terminale elongate and form the cauda equina.
Simultaneously, the lumbar cistern forms as the dura–arachnoid sac separates from the pia mater. At birth, the conus lies at about the L3 vertebral level, and, by adulthood, it reaches about the L1 vertebral level. However, the normal length of the adult spinal cord varies significantly. The conus may extend to the T12 to L3 vertebral levels in normal conditions. The age-related changes in the position of the conus and the formation and enlargement of the cauda equina and lumbar cistern have critical implications for clinical procedures, such as lumbar puncture and the functional outcomes of herniated intervertebral discs .Because the spinal cord is shorter than the vertebral column in adults, the spinal cord segments do not correspond numerically with the vertebrae that lie at the same level.
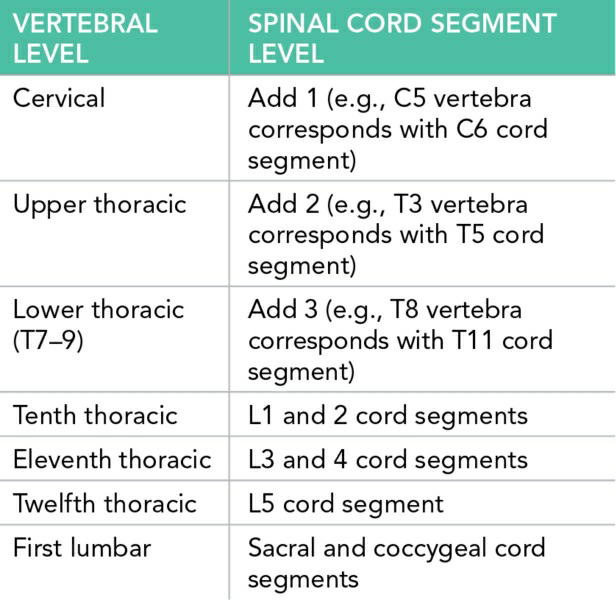
Table 2.7 describes which spinal segment is contiguous with a given vertebral body in adults.
Tethered Spinal Cord
During development, the filum terminale may become abnormally thickened or infiltrated with other tissue. This may produce tension and/or traction on the caudal part of the spinal cord that interferes with the normal
ascent of the cord and results in a low-lying conus medullaris. Such a condition is referred to as tethered cord syndrome (TCS). TCS is associated with multiple possible disorders presenting from the lower back through the pelvis and lower limbs.
Back Muscle Development
All the muscles of the back (except the trapezius) develop from the segmental myotomes. Each myotome splits into two portions, the epimere and the hypomere. The epimere is smaller, forms posterior to the developing vertebral column (in the back of the body), and is innervated by the posterior rami of spinal nerves (Fig. 2.23). The hypomere is larger, forms lateral and anterior to the incipient vertebral column, and is supplied by the anterior rami of spinal nerves. The pharyngeal (branchial) arches in the head region also give rise to numerous muscles, all of which are innervated by cranial nerves.
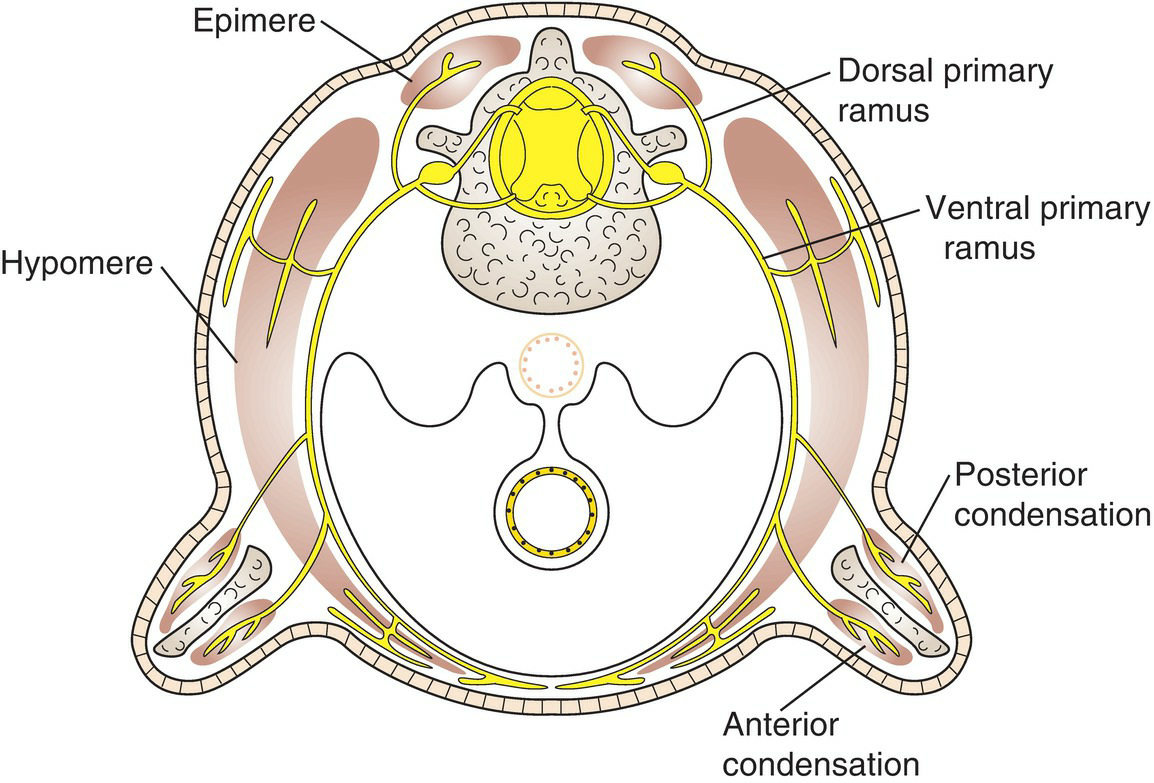
Figure 2.23 Schematic cross section through the thorax and upper limb bud of an embryo showing the relations between the anterior and posterior primary rami of spinal nerves and the hypomere and epimere.
The pattern of innervation seen in the adult reveals the developmental history of the muscles of the back. All the muscles of the superficial and intermediate groups (except for trapezius) are supplied by anterior rami of spinal nerves. All the muscles of the deep group are supplied by posterior rami of spinal nerves.
The trapezius is innervated by cranial nerve XI (spinal accessory nerve). Therefore, the deep muscles originated in the epimeres, the superficial and intermediate muscles (except trapezius)formed from the hypomeres, and the trapezius developed from pharyngeal arches.
The deep group muscles are referred to as the intrinsic muscles of the back because their developmental origins are from the epimeres, within the back proper. The superficial and intermediate group muscles are termed the extrinsic muscles of the back because their origins are from the hypomeres and pharyngeal arches, outside the back proper. Whereas the intrinsic muscles remain in their area of origin, the extrinsic muscles secondarily grow into the back from other sites of origin.
