The digestive tube is formed from the yolk sac. The entoderm forms the epithelial lining, and the splanchnic mesenchyme forms the surrounding muscle and serous coats.
The developing gut is divided into the foregut, midgut, and hindgut (Fig. 7.40).
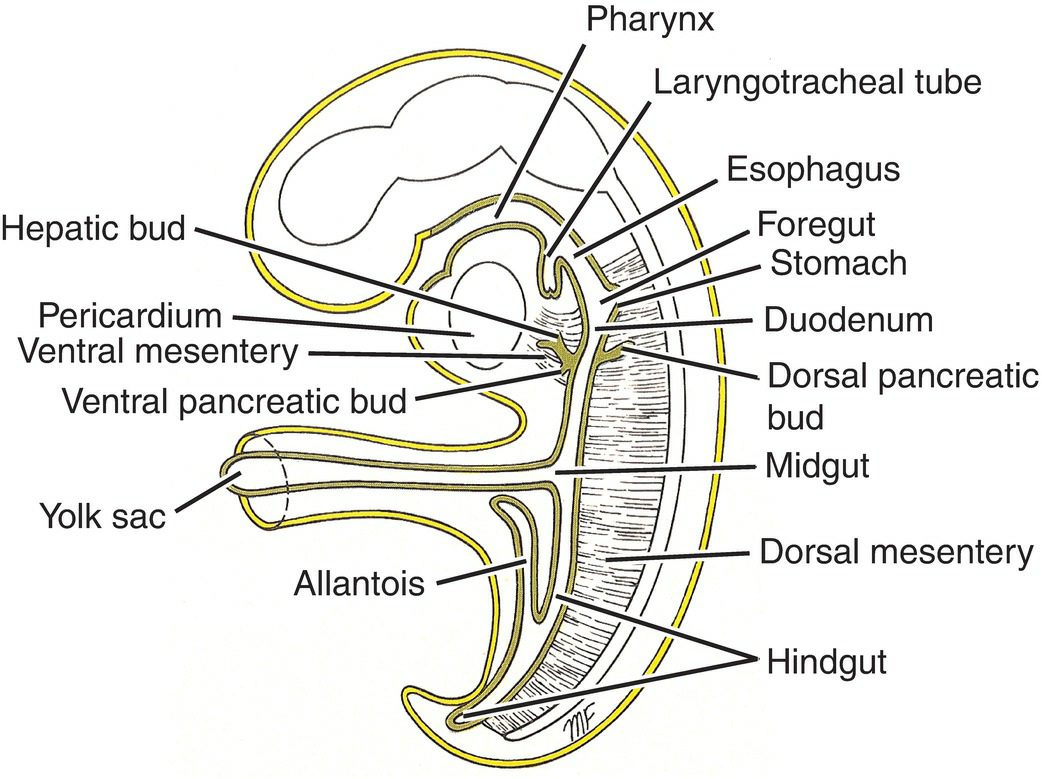
Figure 7.40 The foregut, midgut, and hindgut. The positions ofthe ventral and dorsal mesenteries, the hepatic bud, and the ventraland dorsal pancreatic buds are also shown.
Esophagus Development
The esophagus develops from the narrow part of the foregut that succeeds the pharynx (see Fig. 7.40). At first, it is a short tube, but when the heart and diaphragm descend, it elongates rapidly.
Esophageal Stenosis
Esophageal stenosis is a narrowing of the lumen of the esophagus, which commonly occurs in the lower part. It is treated by dilatation.
Congenital Short Esophagus
Abnormal shortness of the esophagus is caused by an esophageal hiatus hernia in the diaphragm. Stomach contents flow into the esophagus, resulting in esophagitis.
Esophageal Atresia
Atresia of the esophagus, with and without fistula, with the trachea.
Stomach Development
The stomach develops as a dilatation of the foregut (Fig. 7.41). To begin with, it has a ventral and dorsal mesentery. Very active growth takes place along the dorsal border, which becomes convex and forms the greater curvature.
The anterior border becomes concave and forms the lesser curvature. The fundus appears as a dilatation at the upper end of the stomach.
At this stage, the stomach has a right and left surface to which the right and left vagus nerves are attached, respectively. With the great growth of the right lobe of the liver, the stomach is gradually rotated to the right so that the left surface becomes anterior and the right surface posterior.
The ventral and dorsal mesenteries now change position as a result of rotation of the stomach, and they form the omenta and various peritoneal ligaments. The pouch of the peritoneum behind the stomach is known as the lesser sac.
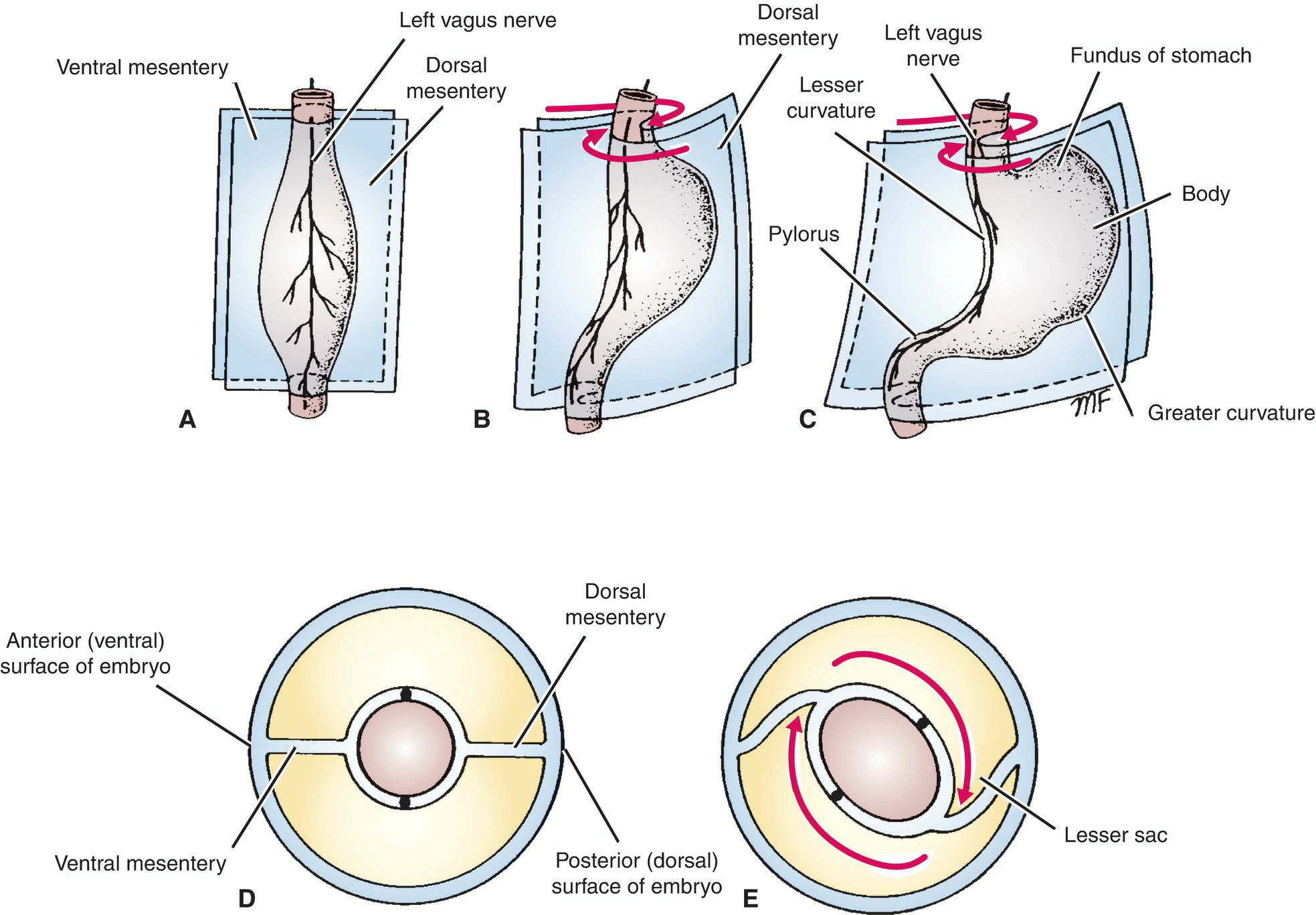
Figure 7.41 Development of the stomach in relation to the ventral and dorsal mesenteries.
A–C. Lateral views of pre-
(A), early
(B),and late
(C) phases of rotation.
D, E. Cross-sectional views of pre-
(D) and mid-phases of rotation.
Note how the stomach rotates sot hat the left vagus nerve comes to lie on the anterior surface of the stomach. Note also the position of the lesser sac.
Congenital Hypertrophic Pyloric Stenosis
Hypertrophic pyloric stenosis is a relatively common emergency in infants between the ages of 3 and 6 weeks. The child ejects the stomach contents with considerable force.
The exact cause of the stenosis is unknown, although evidence suggests that the number of autonomic ganglion cells in the stomach wall is fewer than normal.
This possibility leads to prenatal neuromuscular incoordination and localized muscular hypertrophy and hyperplasia of the pyloric sphincter. It is much more common in male children.
Duodenum Development
The duodenum is formed from the most caudal portion of the foregut and the most cephalic end of the midgut. This region rapidly grows to form a loop. At this time, the duodenum has a mesentery that extends to the posterior abdominal wall and is part of the dorsal mesentery.
A small part of the ventral mesentery is also attached to the ventral border of the first part of the duodenum and the upper half of the second part of the duodenum.
When the stomach rotates, the duodenal loop is forced to rotate to the right, where the second, third, and fourth parts adhere to the posterior abdominal wall.
Now the peritoneum behind the duodenum disappears. However, some smooth muscle and fibrous tissue that belong to the dorsal mesentery remains the suspensory ligament of the duodenum (ligament of Treitz), and this fixes the terminal part of the duodenum and prevents it from moving inferiorly (Fig. 7.42). The liver and pancreas arise as entodermal buds from the developing duodenum.
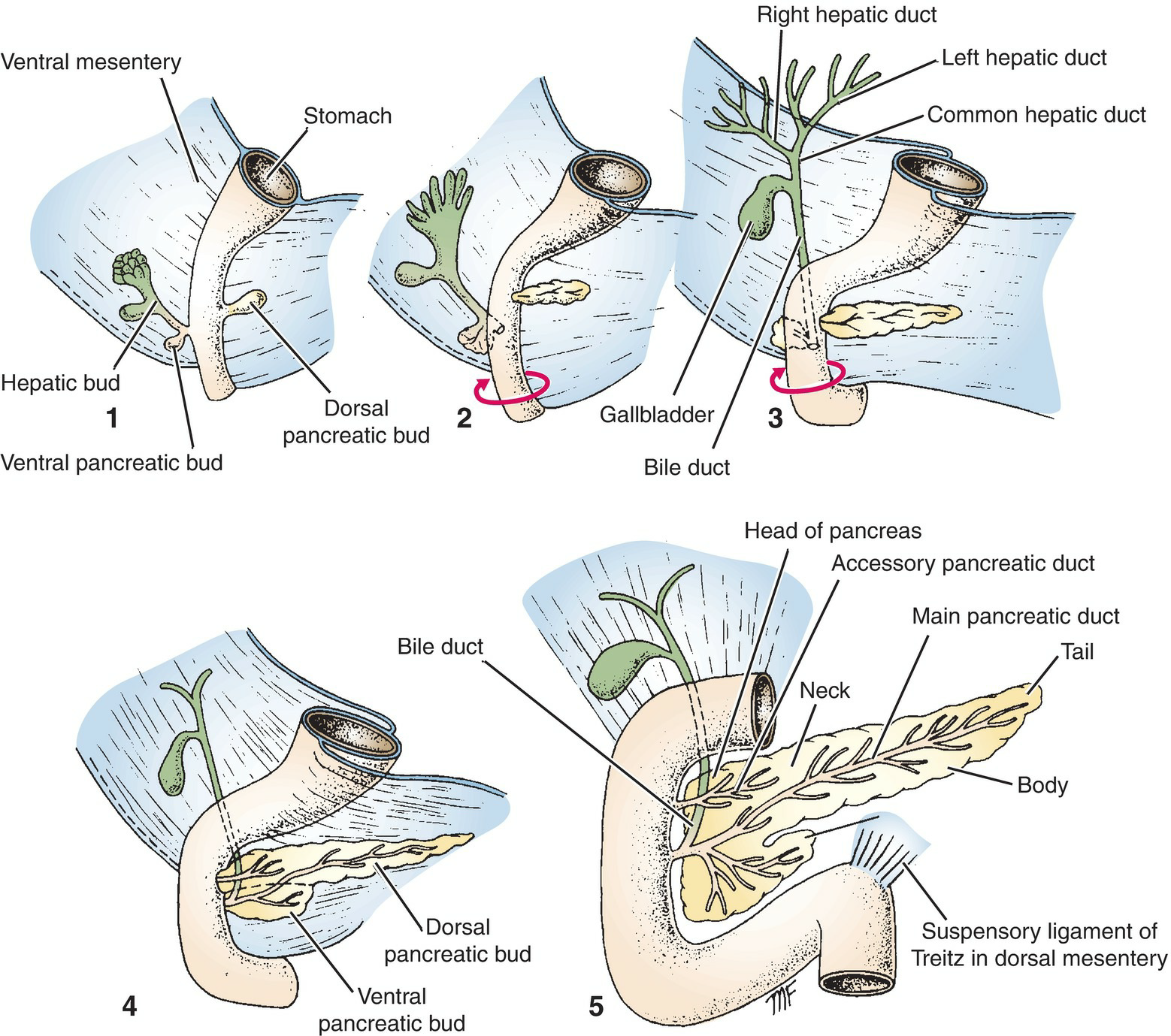
Figure 7.42 Progressive stages (1–5) in development of the pancreas and the extrahepatic biliary apparatus. The red arrows indicate the direction of rotation of the duodenum.
Atresia and Stenosis
During the development of the duodenum, the lining cells proliferate at such a rate that the lumen becomes completely obliterated. Later, as a result of degeneration of these cells, the gut becomes recanalized.
Failure of recanalization could produce atresia or stenosis. Different forms of duodenal atresia and stenosis are shown in Figure 7.43. Vomiting is the most common presenting symptom, and the vomitus usually is bile stained. Surgical treatment during the first few days of life is essential.
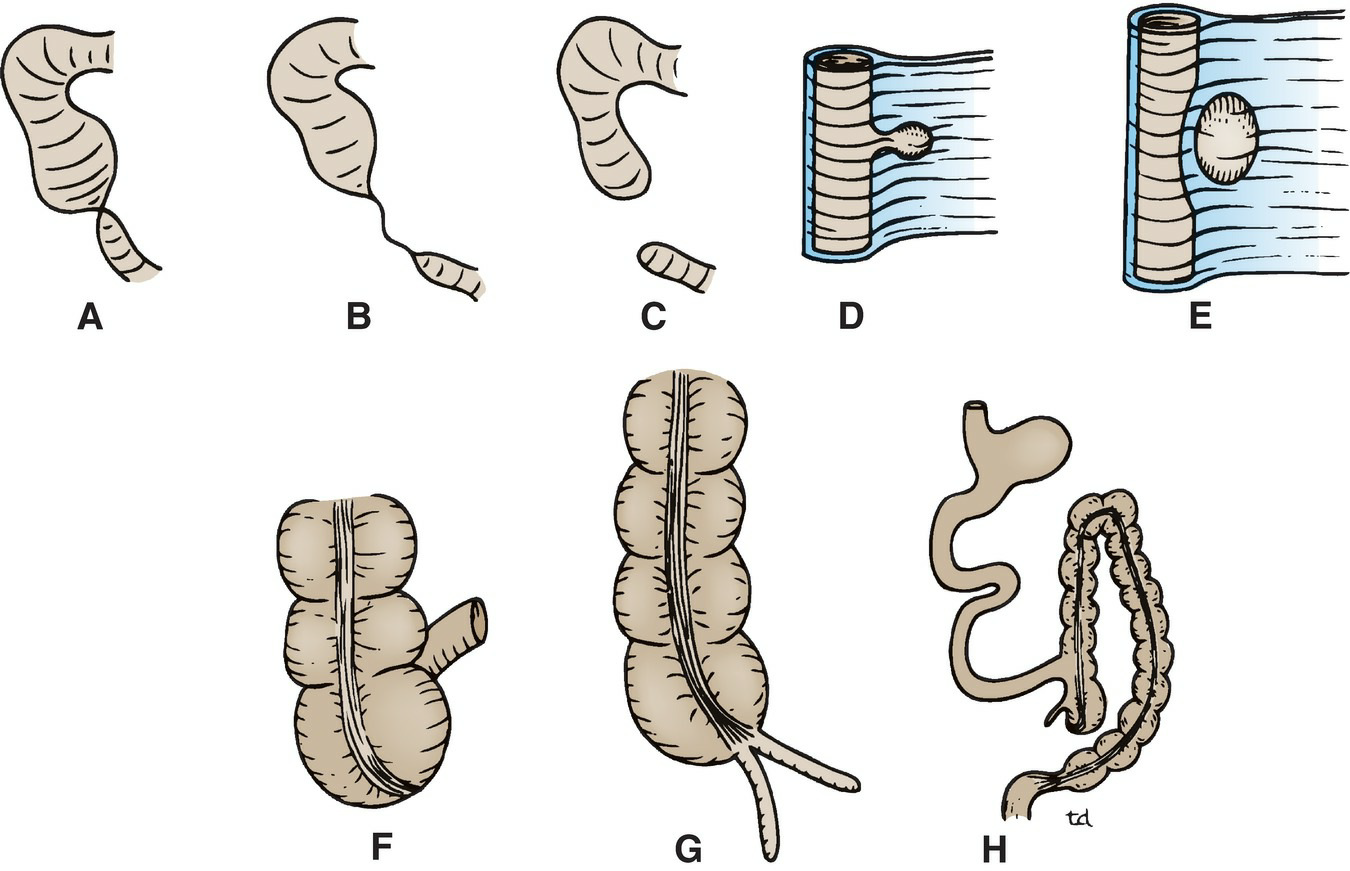
Figure 7.43 Some common congenital anomalies of the intestinal tract.
A–C. Congenital atresia’s of the small intestine.
D. Diverticulum of the duodenum or jejunum.
E. Mesenteric cyst of the small intestine.
F. Absence of the appendix.
G. Double appendix.
H. Malrotation of the gut, with the appendix lying in the left iliac fossa. For Meckel diverticulum, see Figure 6.37.
Midgut Development
The distal duodenum, the jejunum and ileum, and the large intestine as far as the distal third of the transverse colon develop from the midgut. The midgut increases rapidly in length and forms a loop to the apex, on which the vitelline duct is attached. This duct passes through the widely open umbilicus (see Fig. 7.40).
At the same time, the dorsal mesentery elongates, and passing through it from the aorta to the yolk sac are the vitelline arteries. These arteries now fuse to form the superior mesenteric artery, which supplies the midgut and its derivatives. The rapidly growing liver and kidneys now encroach on the abdominal cavity, causing the midgut loop to herniate into the umbilical cord.
A diverticulum appears at the caudal end of the bowel loop, and this forms the cecum. At first, the diverticulum is conical; later, the upper part expands and forms the cecum, where as the lower part remains rudimentary and forms the appendix (Fig. 7.44). After birth, the wall of the cecum grows unequally, and the appendix comes to lie on its medial side.
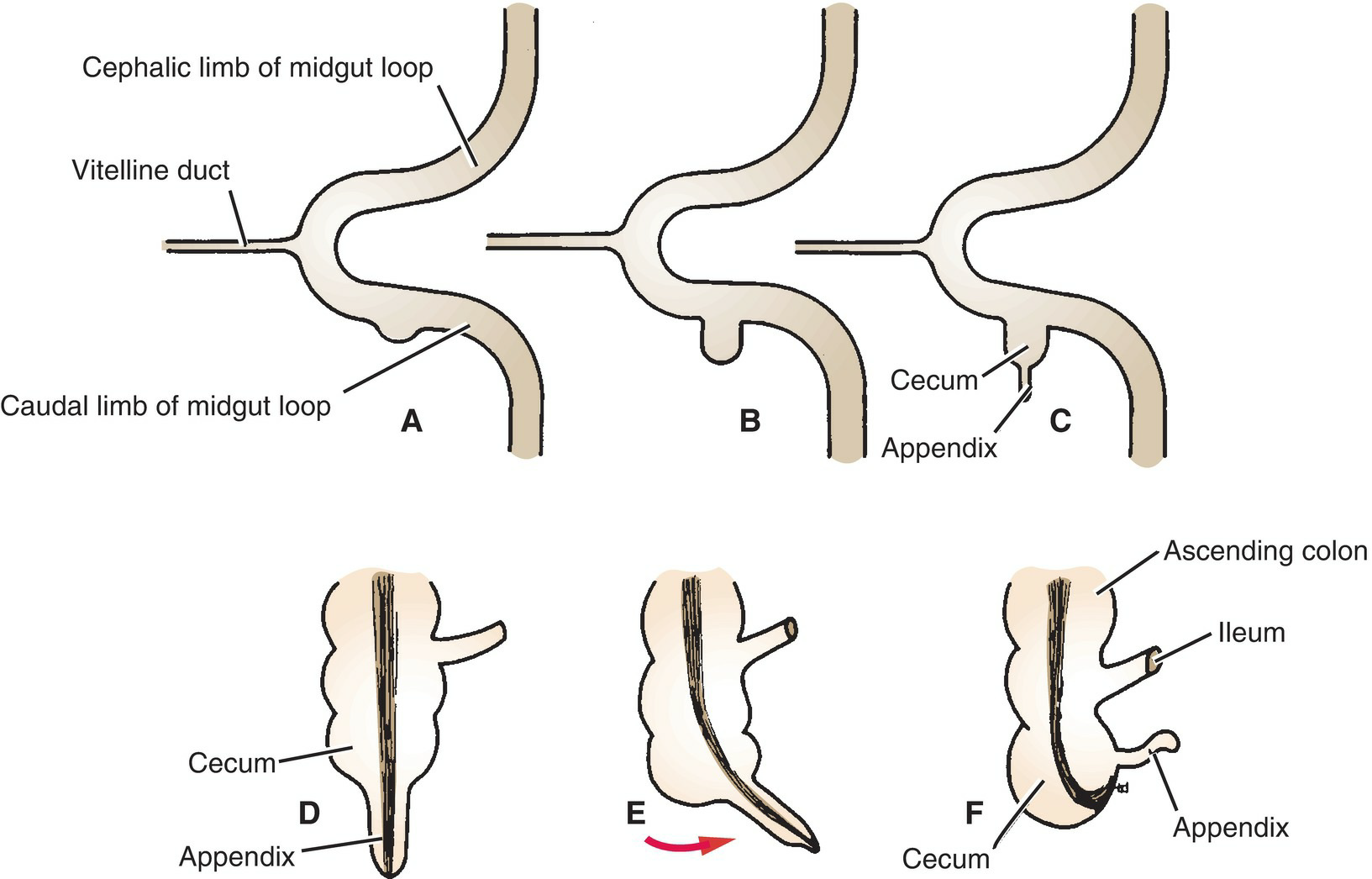
Figure 7.44 Progressive stages (A–F) in development of the cecum and appendix. The red arrow indicates the rotation of the appendix. The final stages of development (stages D, E, and F) take place after birth.
Although the loop of gut is in the umbilical cord, its cephalic limb becomes greatly elongated and coiled and forms the future jejunum and greater part of the ileum. The caudal limb of the loop also increases in length, but it remains uncoiled and forms the future distal part of the ileum, the cecum, the appendix, the ascending colon, and the proximal two thirds of the transverse colon.
Midgut Loop Rotation in the Umbilical Cord and Return to Abdominal Cavity
While in the umbilical cord, the midgut rotates around an axis formed by the superior mesenteric artery and the vitelline duct. Viewing the embryo from the anterior aspect, a counterclockwise rotation of ~90° occurs (Fig. 7.45).
Later, as the gut returns to the abdominal cavity, the midgut rotates counterclockwise an additional 180°. Thus, a counterclockwise rotation of a total of 270° has occurred (Fig. 7.46).
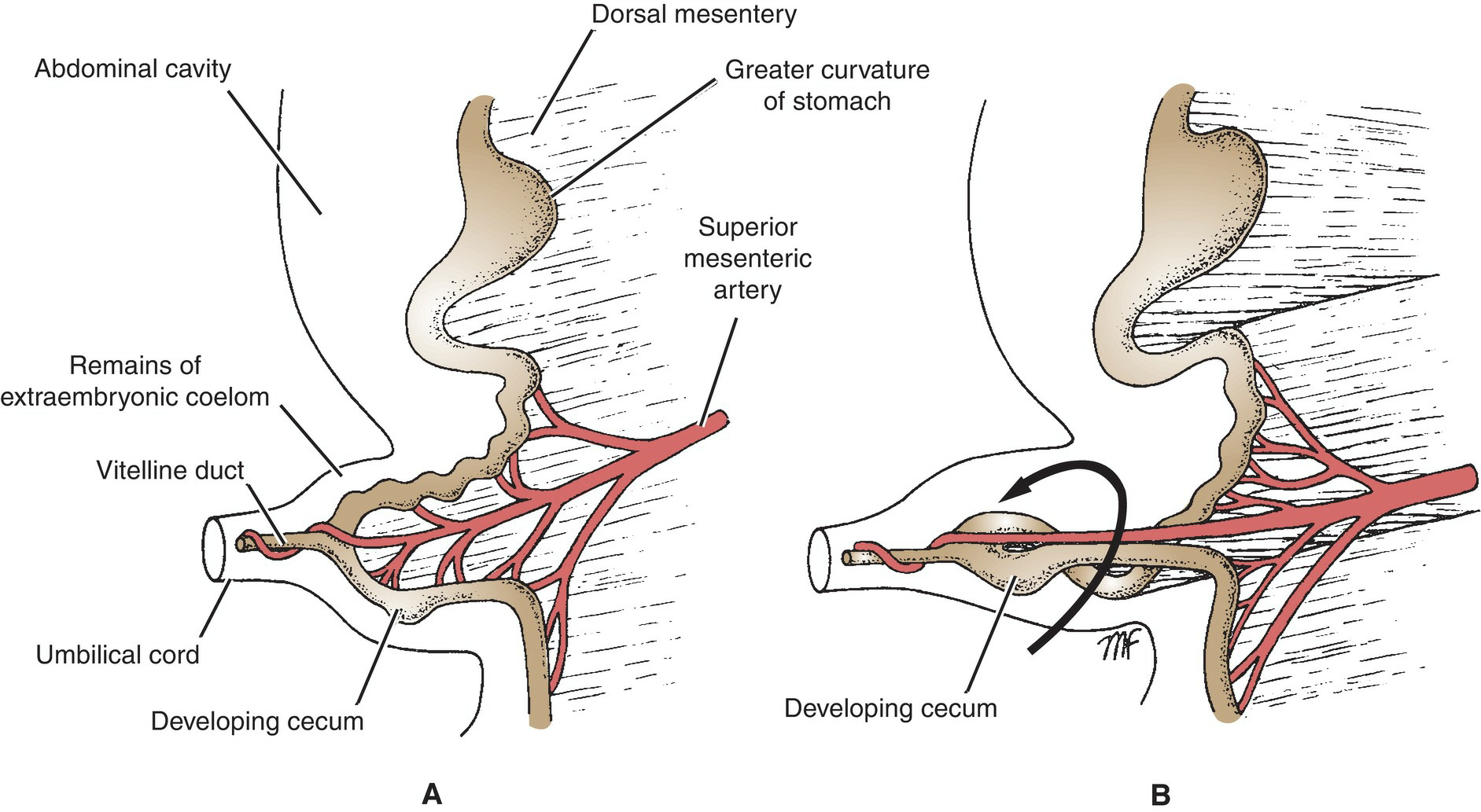
Figure 7.45 Left-side views of the midgut loop before rotation(A) and during initial counterclockwise 90° rotation (B) while it is in the extraembryonic coelom in the umbilical cord.
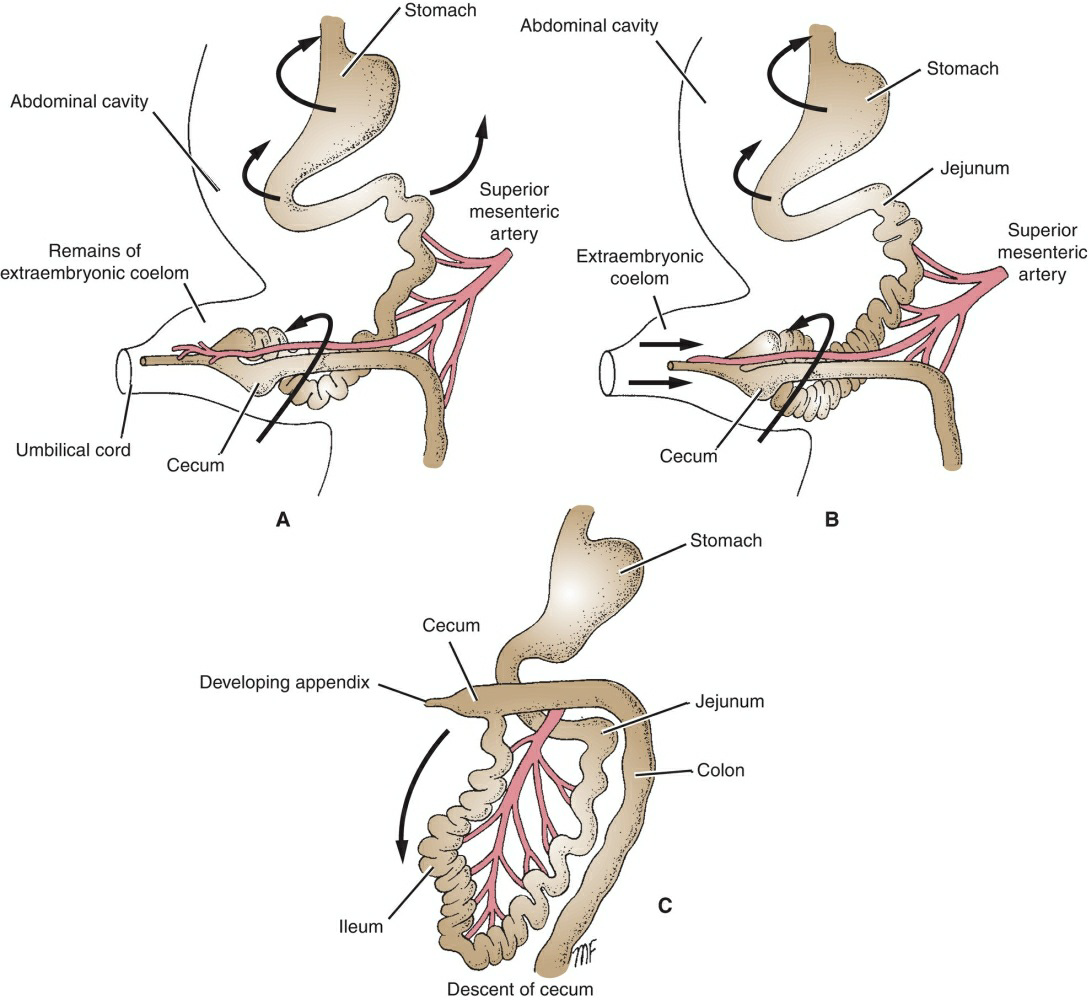
Figure 7.46 A, B. Left-side views of the counterclockwise 180° rotation of the midgut loop as it is withdrawn into the abdominal cavity. C. The descent of the cecum takes place later.
The rotation of the gut results in part of the large intestine (transverse colon) coming in front of the superior mesenteric artery and the second part of the duodenum; the third part of the duodenum comes to lie behind the artery.
The cecum and appendix come into close contact with the right lobe of the liver. Later, the cecum and appendix descend into the right iliac fossa so that the ascending colon and right colic flexure are formed. Thus, the rotation of the gut has resulted in the large gut coming to lie laterally and encircle the centrally placed small gut. The primitive mesenteries of the duodenum and ascending and descending colons now fuse with the parietal peritoneum on the posterior abdominal wall.
This explains how these parts of the developing gut become retroperitoneal. The primitive mesenteries of the jejunum and ileum, the transverse colon, and the sigmoid colon persist as the mesentery of the small intestine, the transverse mesocolon, and the sigmoid mesocolon, respectively.
The rotation of the stomach and duodenum to the right is largely brought about by the great growth of the right lobe of the liver. The left surface of the stomach becomes anterior, and the right surface becomes posterior. A pouch of peritoneum becomes located behind the stomach and is called the lesser sac.
Vitelline Duct Fate
The midgut is at first connected with the yolk sac by the vitelline duct. By the time, the gut returns to the abdominal cavity, the duct becomes obliterated and severs its connection with the gut.
Hindgut Development
The left colic flexure, descending colon, sigmoid colon, rectum, and upper half of the anal canal are developed from the hindgut.
Intestinal Diverticula
All coats of the intestinal wall are found in the wall of a congenital diverticulum. In the duodenum, diverticula are found on the medial wall of the second and third parts (see Fig. 7.43). Usually, these are symptomless.
Jejunal diverticula occasionally occur and usually give rise to no symptoms. A diverticulum of the cecum is commonly situated on the medial side of the cecum close to the ileocecal valve. It may be subject to acute inflammation and then is confused with appendicitis. Diverticula of the colon are acquired, not congenital.
Intestinal Atresia and Stenosis
The most common site of an atretic or stenotic obstruction is in the duodenum . The next most common sites are the ileum and jejunum, respectively (see Fig. 7.43). Frequently, the obstruction occurs at multiple sites. The cause is possibly the failure of the lumen to become recanalized after it has been blocked by epithelial proliferation of the cells of the mucous membrane. Other causes have been suggested, such as vascular damage associated with twisting or volvulus of the intestine.
Persistent bile-stained vomiting occurs from birth. Surgical relief of the obstruction should be carried out as soon as possible.
Digestive System Duplication
In duplication of the digestive system, the normal degeneration of the mucous membrane cells, which have proliferated to temporarily block the lumen, occurs at two sites simultaneously instead of at one. In this way, two lumina are formed side by side. The additional segment of bowel should be removed as soon as possible, because it may cause obstruction or be the site of hemorrhage or perforation.
Complete Absence of Rotation or Incomplete Rotation of Midgut Loop
The complete absence of rotation is rare. In cases of in complete rotation, no further rotation occurs after the initial counterclockwise rotation of 90° in the umbilical cord. Thus, the duodenum, jejunum, and ileum remain on the right side of the abdomen, and the cecum and colon are on the left side of the abdomen (see Fig. 7.43). In other cases, a counterclockwise rotation of 180° occurs, and although the duodenum may take up its correct position posterior to the superior mesenteric artery, the cecum comes to lie anterior and to the left of the duodenum. Abnormal adhesions form, which run across the anterior surface of the duodenum and cause obstruction to its second part.
Midgut Loop Malrotation
Counterclockwise rotation of 90° followed by clockwise rotation of 90° or 180° may occur. In these cases, the duodenum comes to lie anterior to the superior mesenteric artery, and the colon may come to lie anterior to the mesentery of the small intestine. Repeated vomiting is usually the presenting symptom and is caused by duodenal obstruction. Surgical correction of the incomplete rotation or malrotation of the gut is performed, and all adhesions are divided.
Persistence of the Vitellointestinal Duct
The vitelline duct in the early embryo connects the developing gut to theyolk sac (Fig. 7.47). Normally, as development proceeds, the duct is obliterated, severs its connection with the intestine, and disappears. Persistence of the vitellointestinal duct can result in an umbilical fistula (see Fig. 6.37). If the duct remains as a fibrous band, a loop of the small intestine can become wrapped around it, causing intestinal obstruction.
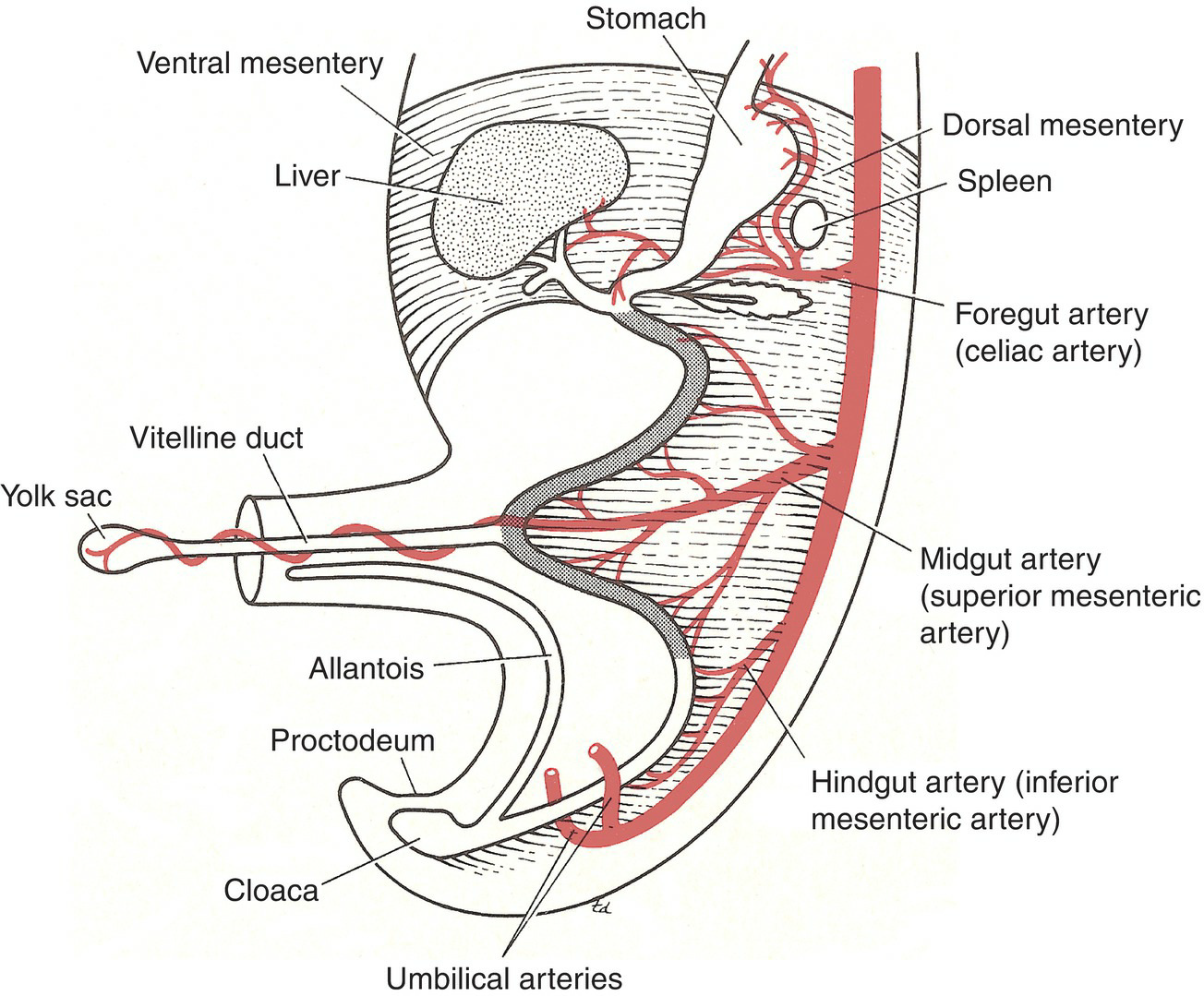
Figure 7.47 Formation of the midgut loop (shaded). Note how the superior mesenteric artery and the vitelline duct form an axis for the future rotation of the midgut loop.
Meckel Diverticulum
Meckel’s diverticulum, a congenital anomaly, represents a persistent portion of the vitellointestinal duct. The diverticulum is located on the antimesenteric border of the ileum about 2 ft (61 cm) from the ileocecal junction. It is about 2 in. (5 cm) long and occurs in about 2% of individuals. The diverticulum is important clinically, because it may possess a small area of gastric mucosa, and bleeding may occur from a “gastric” ulcer in its mucous membrane. Moreover, the pain from this ulcer may be confused with the pain from appendicitis. Should a fibrous band connect the diverticulum to the umbilicus, a loop of small bowel may become wrapped around it, causing intestinal obstruction.
Undescended Cecum and Appendix
In cases of undescended cecum and appendix, an inflammation of the appendix would give rise to tenderness in the right hypochondrium, which may lead to a mistaken diagnosis of inflammation of the gallbladder.
Appendiceal Anomalies
Agenesis of the appendix (failure to develop) is extremely rare; however, a few examples of double appendix have been reported (see Fig. 7.43). The possibility of left-sided appendix in individuals with transposition of thoracic and abdominal viscera or in cases of arrested rotation of the midgut should always be remembered.
Colon Anomalies
The congenital anomaly of undescended cecum or failure of rotation of the gut so that the cecum lies in the left iliac fossa may give rise to confusion in diagnosis. The pain of appendicitis, for example, although initially starting in the umbilical region, may shift not to the right iliac fossa, but to the right upper quadrant or to the left lower quadrant.
