The male sex chromosome causes the genital ridge to secrete testosterone and induces the development of the testis and the other internal and external organs of reproduction.
The sex cords of the genital ridge become separated from the coelomic epithelium by the proliferation of the mesenchyme (Fig. 6.30).
The outer part of the mesenchyme condenses to form a dense fibrous layer, the tunica albuginea. The sex cords become U shaped and form the seminiferous tubules. The free ends of the tubules form the straight tubules, which join one another in the mediastinum testis to become the rete testis.
The primordial sex cells in the seminiferous tubules form the spermatogonia, and the sex cord cells form the Sertoli cells. The mesenchyme in the developing gonad makes up the connective tissue and fibrous septa.
The interstitial cells, which are already secreting testosterone, are also formed of mesenchyme. The rete testis becomes canalized, and the tubules extend into the mesonephric tissue, where they join the remnants of the mesonephric tubules; the latter tubules become the efferent ductless of the testis. The mesonephric duct forms the duct of the epididymis, the vasdeferens, the seminal vesicle, and the ejaculatory duct (see Fig. 6.30).
Testicular Descent
The testis develops high up on the posterior abdominal wall, and in late fetal life, it “descends” behind the peritoneum, dragging its blood supply, nerve supply, and lymphatic drainage after it.
Congenital Anomalies
The testis may be subject to the following congenital anomalies. Anterior inversion, in which the epididymis lies anteriorly and the testis and the tunica vaginalis lie posteriorly.
Polar inversion, in which the testis and epididymis are completely inverted.
Imperfect descent (cryptorchidism): Incomplete descent (Fig. 6.31), in which the testis, although traveling down its normal path, fails to reach the floor of the scrotum. It may be found within the abdomen, within the inguinal canal, at the superficial inguinal ring, or high up in the scrotum.
Maldescent (Fig. 6.32), in which the testis travels down an abnormal path and fails to reach the scrotum. It may be found in the superficial fascia of the anterior abdominal wall above the inguinal ligament, in front of the pubis, in the perineum, or in the thigh. The testes must leave the abdominal cavity because the temperature there retards the normal process of spermatogenesis.
If an incompletely descended testis is brought down into the scrotum by surgery before puberty, it will develop and function normally. A mal descended testis, although often developing normally, is susceptible to traumatic injury and, for this reason, should be placed in the scrotum.
Many authorities believe that the incidence of tumor formation is greater in testes that have not descended into the scrotum. The appendix of the testis and the appendix of the epididymis are embryologic remnants found at the upper poles of these organs that may become cystic.
The appendix of the testis is derived from the paramesonephric ducts, and the appendix of the epididymis is a remnant of the mesonephric tubules.
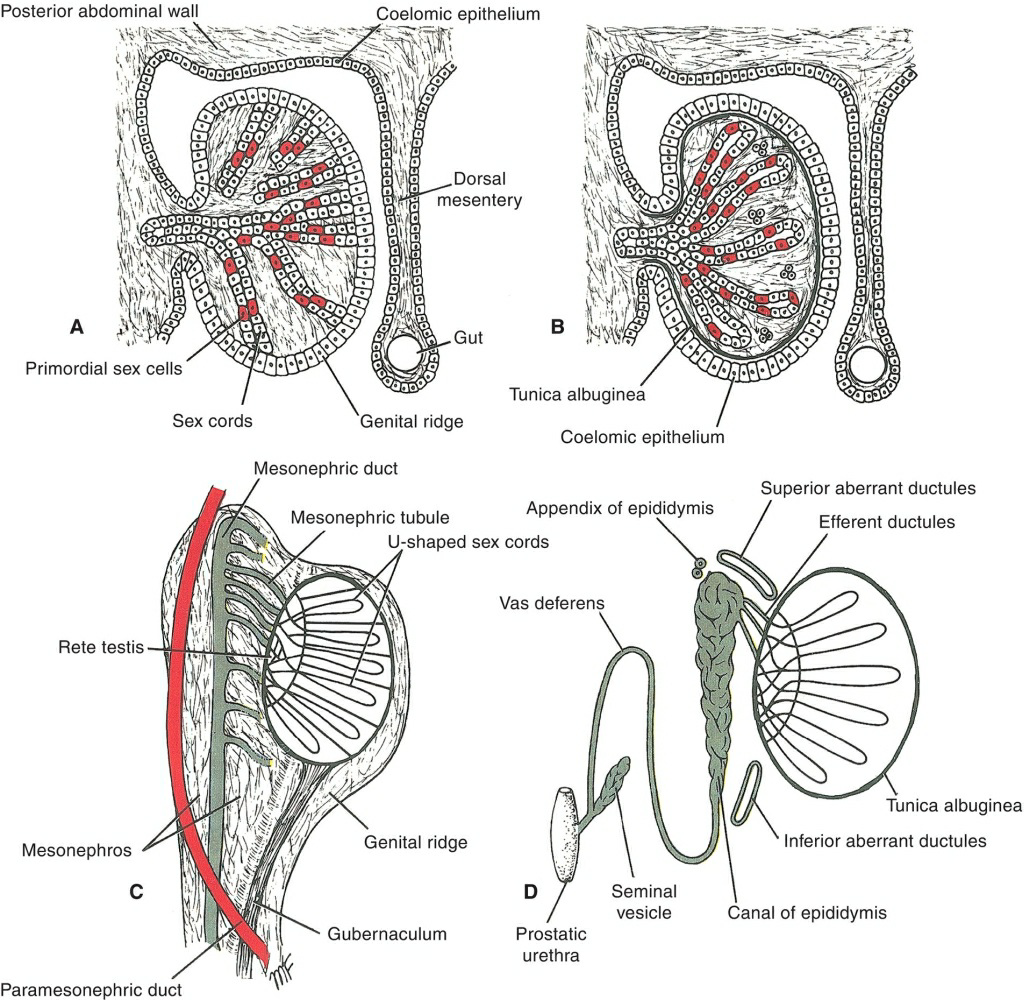
Figure 6.30 The formation (A), development (B,C), and fate (D) of the testis and its ducts.
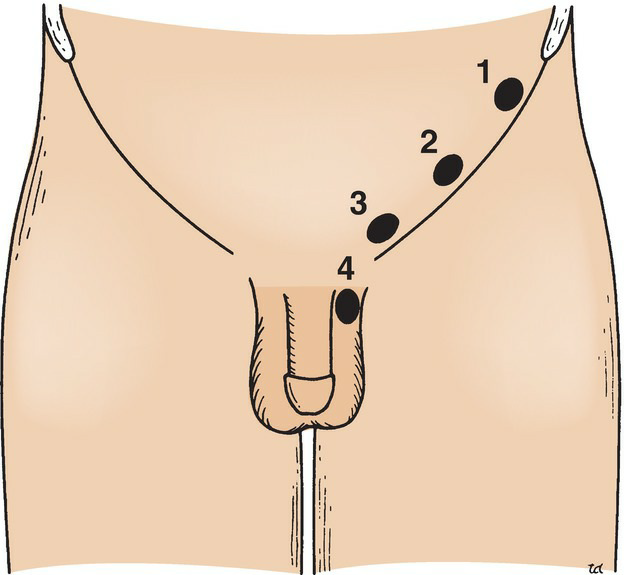
Figure 6.31 Four degrees of incomplete descent of the testis. (1) In the abdominal cavity close to the deep inguinal ring. (2) In the inguinal canal. (3) At the superficial inguinal ring. (4) In the upper part of the scrotum.
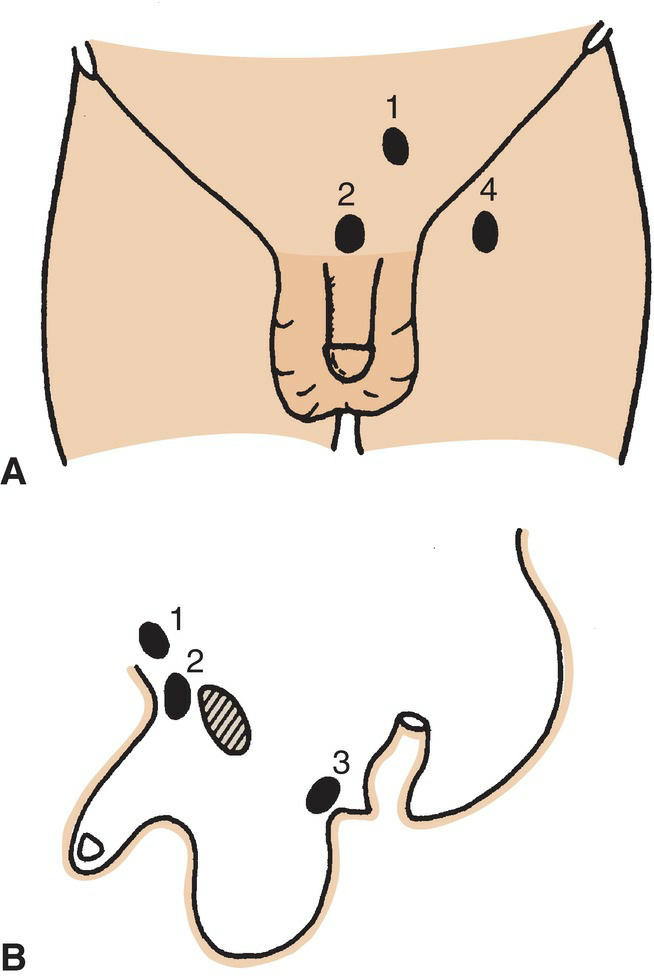
Figure 6.32 Four types of maldescent of the testis. A. Anterior view. B. Sagittal section. (1) In the superficial fascia of the anterior abdominal wall, above the superficial inguinal ring. (2) At the root of the penis. (3) In the perineum. (4) In the thigh.
